FNOL/FROI Setup
Use Roots to reduce claims leakage and reach 90%+ STP goals for claims setup
Roots automates the entire FNOL/FROI process with our AI Agent relieving your claims staff from monotonous administrative tasks, leading to increased productivity and faster claims handling cycle times.

Top insurance companies trust Roots
























With automated FNOL setup, you can increase your team's capacity to avoid backlogs and overcome seasonal or unforeseen incidents. Automatically monitor email inboxes, attachments, mailrooms, and online platforms for new claim correspondence. Quickly classify new claims documents without requiring manual review. In fact, a leading insurance carrier processes 99% of all FNOL correspondence straight-through using Roots.
Reduce claims cycle times by processing claims more quickly, with a 90% reduction in manual intervention for claim setup. Let the Roots claims setup AI Agent extract essential data points and automate claims lookup to identify whether a claim already exists or if a new claim should be filed. Create acknowledgment letters for adjusters to evaluate and send out.
Error-free data speeds up claim processes and helps to reduce potential overpayment. Roots gives your adjusters a break from tedious data extraction and automatically identifies all the crucial data points like claimant name, policy number, claim amount, and claim date. We can even add claim data into the proper systems and record.
CHALLENGE
Quarter-end peaks and seasonal events overwhelm your claims teams, leading to employees working longer hours, and increased leakage
Historically, First Notice of Loss (FNOL) and First Report of Injury (FROI) require really manual steps, which have an impact on efficiency and accuracy. Claims documents, which range from organized forms to police reports, medical records and photos, received via multiple submission channels. Extracting data from these sources requires takes adjusters’ time. Busy seasons and NATCAT events add to the problems and can overburden claims teams, resulting in the need for temporary staffing, delayed processing, and greater premium leakage. However, there is a better FNOL/FROI setup solution.
The Power of AI and FNOL/FROI Setup
The Roots AI Agent receives, processes, checks for duplicate claims, and handles FNOL correspondence faster and more accurately than manual approaches. Give your claims team an AI-powered digital assistant to overcome capacity constraints, particularly during seasonal or unforeseen occurrences, and let your highly skilled employees focus on claims handling, adjudication, and client engagement.
Insurance AI Agents Support Across Business Lines
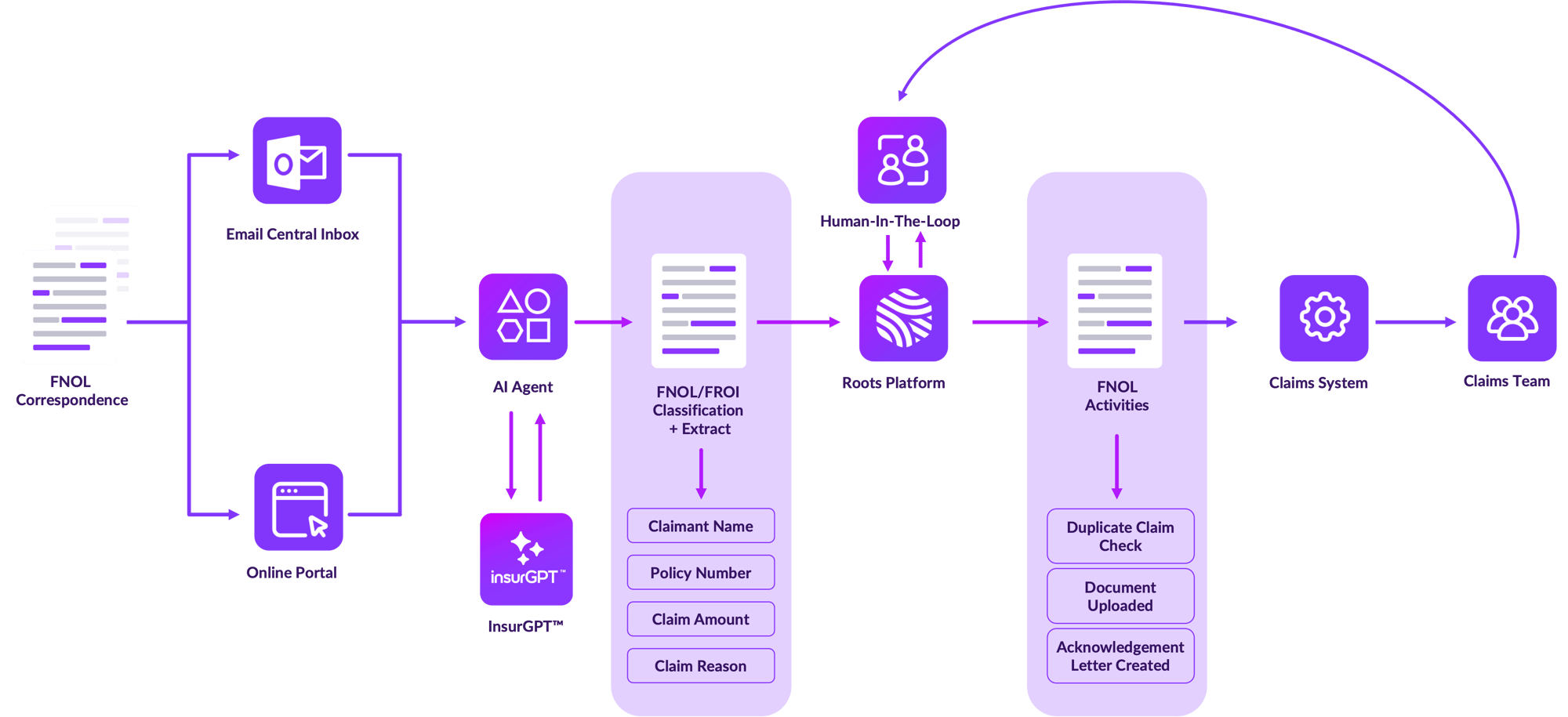
How It Works
How Automated First Notice of Loss (FNOL) and First Report of Injury (FROI) Setup Works?
Monitor
Watch email inboxes, attachments, mailrooms, or online systems automatically looking for FNOL/FROI correspondence.
Classify
The Roots Platform classifies each document in the FNOL package.
Extract
Identify all the crucial data points like claimant name, policy number, claim amount, and claim date.
Existing Claim Check
Automatic look up determines if it is an existing claim or if a new claim should be created.
Data Input
Claim data is automatically added to the appropriate systems and record.
Notice to Claimant
The Platform drafts an acknowledgment letter for an adjuster to review.
BENEFITS
Eliminate backlogs and take control of claim setup process with Roots

- Process claims faster with a 90% reduction in manual intervention for claims setup.
- Add scalability to your team to overcome capacity issues, especially during seasonal or unforeseen events.
- Improve straight-through processing (STP) with 99% of all FNOL correspondence handled automatically.
- Improve efficiency and automate the end-to-end FNOL and FROI processes freeing up claims team members from administrative tasks.
- Increase data accuracy and identify missing or incorrect claims data to reduce delays.



